Symposium focus: Encouraging more women to train as Oral and Maxillofacial surgeons12 min read
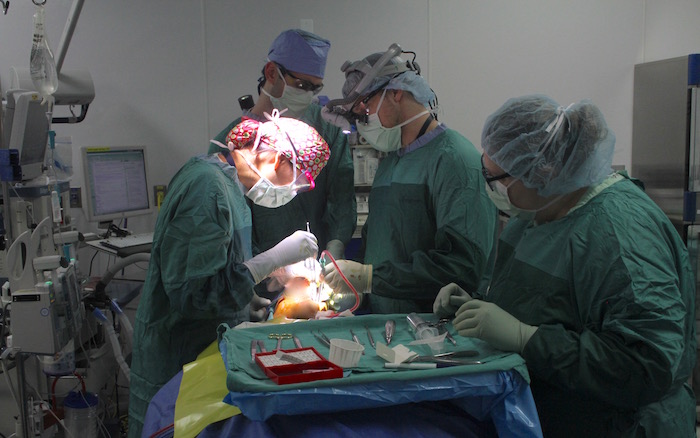
Ann Arbor, Mich., Jan. 29, 2019 -– Dr. Justine Moe projects quiet confidence and efficiency as she leads a jaw surgery early on a Thursday morning in Operating Room 30 at the University of Michigan medical center.
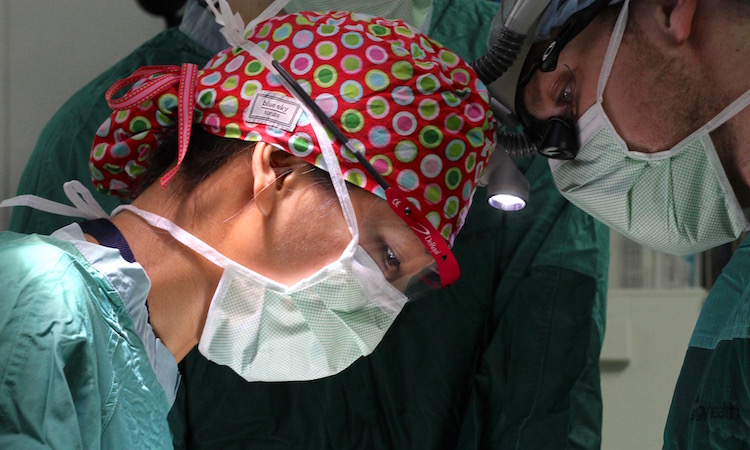
Leaning down close over the patient’s face and wide-open mouth, Moe is focused on removing a tumor on the left mandible. Her assisting surgeon, Dr. Jake Peterson, stands on the opposite side of the patient, next to a scrub technician who hands them the surgical instruments they request. A nurse anesthetist follows the patient’s vital signs on nearby monitors while OR nurses and various assistants enter and exit the room as needed. A School of Dentistry student observes the procedure from the head of the operating table.

This is a surgery that can be fairly straightforward or one that can be seriously complicated if the surgeon finds evidence of cancer or other problems when the area around the tumor is examined. As Moe resects the mass and surrounding tissue, they are placed in a plastic bottle and taken immediately to the hospital’s pathology lab. About 15 minutes later, a cell phone chirps on a nearby table. A nurse answers and says it is the pathologist calling to report his findings. Moe steps away from the patient and the nurse holds the phone close to Moe’s face so that Moe won’t have to touch the phone with her surgical gloves. After a brief back-and-forth conversation comparing Moe’s surgical observations with the pathologist’s microscopic findings, Moe returns to the surgery. It is good news for the patient; there doesn’t appear to be cancer cells in the tumor or surrounding tissue.
Moe and Peterson finish repairing the tissue where the tumor was located and suture the incision closed. After nearly an hour of countless critical decisions linked to precise hand movements, Moe’s work is complete and she leaves the OR. In an adjacent room, she lowers her surgical mask and says the procedure went well.
What makes this particular surgery more than just routine, however, is that it was conducted by a female oral and maxillofacial (OMF) surgeon. Across the country, women make up only about 7 percent of the active members of the American Association of Oral and Maxillofacial Surgeons. The gender discrepancy is found in all areas of surgery — only about 19 percent of U.S. surgeons are women — but the shortage of women in oral and maxillofacial surgery (OMFS) is especially significant. There are even fewer female head and neck oncology-trained OMF surgeons; Moe is one of less than 10 in the country. It’s a gap that the U-M is addressing by again hosting a national symposium this year to examine the reasons and solutions. Moe is the lead organizer for the second annual event in early March.

Dr. Brent Ward, chair of dental school’s OMFS/Hospital Dentistry department, identified the gender gap as one of his priorities two years ago when the department celebrated its 100th anniversary and looked ahead to the next century. The longstanding male-dominated profession needs to change, he says, and the first annual symposium last year was an important step in calling attention to the problem. “Our efforts have generated considerable interest and brought focus not only to Michigan as ‘leaders and best,’ but also helped promote a broader and far more robust conversation at other universities and in national organizations,” said Ward, who is also section head of OMFS within the Surgery Department at the U-M medical school.
A significant factor in the gender disparity is that for much of the last century few women applied to or were accepted into dental schools, and the pool of potential OMF surgeons reflected that. It’s only been in about the last 15 years that women now comprise close to 50 percent of dental school students and graduates nationally. Another factor is the rigorous and expensive path to becoming an OMF surgeon. Candidates first need to graduate from dental school with a DDS degree, then complete a residency in OMF, which can include medical school. It is a commitment of at least four to six years. Then there might be a fellowship in a specialty that adds even more time and educational debt for the doctor. Newly graduated dentists may prefer to begin practicing — and paying off their school debt — immediately rather than extend their education by several years. Yet another factor is that new DDS grads, who are usually in their mid- to late-20s, may want to start a family and believe it will be difficult while in an extended training program.
Adding to the equation is that elite residency programs like the one at U-M are highly selective. U-M admits only three OMFS residents (out of about 100 applicants) each year, so there are only 18 residents in the six-year program. For decades, it was common for all the residents to be men. Today the U-M program has three female residents out of 18, the most at one time in the history of the 100-year program. That’s 16 percent or just above the national training program average of 15 percent, which has been inching up in recent years, a hopeful sign.
The educational background of Moe, who was hired last August as a Clinical Assistant Professor in the OMFS/Hospital Dentistry department, is an example of the lengthy journey required for OMF surgeons. A native of Edmonton, Alberta, Canada, she earned her DDS at the Dalhousie University School of Dentistry in Halifax, Nova Scotia. She graduated from Emory University School of Medicine in Atlanta, Ga., and completed internships at the University of California-Los Angeles and at Emory. She obtained her residency in OMFS at Emory and completed a fellowship in Head and Neck Oncologic and Microvascular Surgery at U-M. As part of her U-M faculty appointment, she is also Associate Director of the Head and Neck Oncologic and Microvascular Reconstructive Surgery Fellowship in the Michigan Medicine Department of Surgery, Section of OMFS. (U-M’s OMF surgeons have joint appointments with the School of Dentistry and Michigan Medicine.) Moe specializes in the treatment of head and neck cancer and non-cancerous tumors. Her clinical practice focuses on the comprehensive rehabilitation for facial deformities and tumor resection surgeries, including microvascular reconstructive surgery, dental implant rehabilitation and facial cosmetic procedures.
“Our recruitment of Dr. Moe, who leads this year’s symposium organization, is an example of our success in attracting the best and brightest future stars of our profession to join our team in this and all of our missions,” Ward said. “She and our other faculty and residents — male and female — are committed to taking these efforts to the next level with the symposium as one representation of that commitment.”
Moe said she expects attendance at this year’s symposium, set for the Rackham Building March 8-9, to more than double the 70 participants who attended last year. Participants from around the country and Canada have registered for the presentations and panel discussions. Topics include leadership styles, personal wellness and work-life balance, avoiding burnout, mentorship and networking, conducting effective meetings, conflict management and contract negotiation, among others. Symposium speakers are from medical centers and dental schools from coast to coast, including those in Georgia, Massachusetts, Ohio, Pennsylvania, New Mexico, Oregon, Louisiana and Michigan.
Picking up on a topic that generated considerable discussion at last year’s symposium, Moe cites mentoring as crucial in helping expand the number of female dentists going into OMFS. It’s important for young women considering oral surgery or for those early in their careers to have the resource of other women who have successfully navigated a similar professional course, she said. “What stood out to me throughout my training was the lack of mentors in the field who were women,” Moe said. “I had very impactful role models, but most were male.”
“Effective mentors are so vital in dental and surgical education,” she said. “Not only do mentors bring academic knowledge, surgical experience and knowledge of the specialty, but they also show you how to be a well-rounded and ethical person and practitioner, provide leadership advice and can help you create a fulfilling career.”
Moe initially chose OMFS as her profession because she enjoyed the mix of solving dental problems and the patient’s larger medical needs, and the precision and technicality of the procedures. “An oral and maxillofacial surgeon needs to treat her patients not just for their needs within the oral cavity but comprehensively as a person with coexisting medical illnesses, social needs and personal goals and wishes,” she said.
Moe and her fellow OMF surgeons treat patients who suffer from an incredible range of needs. One day it may be a trauma emergency for someone who has broken their jaw and suffered severe facial lacerations in a fall or traffic accident. Osteomyelitis, or bone infection of the jaws, can require jaw resection and reconstruction with bone grafts and reconstruction plates. Oral cancers often require surgery by OMF surgeons including excision and reconstruction using muscle, bone or skin flaps from other parts of the body. Jaws damaged by cancer or other trauma can be reconstructed using a fibula, the smaller of the two bones in the lower leg. Facial reconstruction is not only vital for the patient’s chewing, eating and talking, but it is important on a cosmetic level as well. Another important consideration in cancer care is dental rehabilitation; teeth are often removed during cancer surgeries and OMF surgeons can place dental implants to replace these teeth. Advances in technology and surgery are constant, Moe notes. She has pioneered using in-house 4-dimensional surgery planning and 3-D printers to create physical models exactly like the patient’s jaws, teeth and other parts of the oral cavity. She can then pre-plan and more accurately predict the nuances of reconstructive surgery.
Moe acknowledges that the training is at times intense, but she counsels women considering oral and maxillofacial surgery that the profession offers a fulfilling career with good work-life balance. “The training process is rigorous, but a career in oral surgery can be very, very rewarding,” she said. “The broad scope of practice that you gain in residency gives you the ability to mold your career to suit your interests, whether it is in trauma, temporomandibular joint surgery, orthognathic surgery, implantology, cancer, cosmetics or dentoalveolar surgery. In particular, academic oral and maxillofacial surgery practice can be a very enriching career for a woman and can allow for a good balance between professional life and personal life.”
The greatest reward is in helping patients through what can be exceptionally difficult times in their lives. “The diagnosis of head and neck cancer can be devastating and terrifying,” Moe said. “As caregivers, we serve as patient advocates from day one and walk along side our patients as they go through this process, often including surgery followed by radiation and chemotherapy, to becoming cancer-free. Sometimes, we prepare patients for end of life, too, and make that more comfortable and not as scary. You have to really listen to patients and understand their goals and wishes, because cancer care is individual and personal. I learn from my patients every day.”
Moe is one of the speakers who will share her insights at the symposium March 8-9. It is open to dental students, medical students, dental and oral surgery residents, staff, academic and private practice oral surgeons, men and women alike — anyone interested in participating in the discussion. “Through this conference, we plan to provide a platform for networking and mentorship among female oral surgeons, for discussion of topics specific to female surgeons and to offer sessions focused on effective leadership skills,” Moe said. Interest has been so strong that registration was temporarily closed last week due to reaching maximum capacity, although anyone interested in the symposium can find additional information on the event website.
###
The University of Michigan School of Dentistry is one of the nation’s leading dental schools engaged in oral health care education, research, patient care and community service. General dental care clinics and specialty clinics providing advanced treatment enable the school to offer dental services and programs to patients throughout Michigan. Classroom and clinic instruction prepare future dentists, dental specialists and dental hygienists for practice in private offices, hospitals, academia and public agencies. Research seeks to discover and apply new knowledge that can help patients worldwide. For more information about the School of Dentistry, visit us on the Web at: www.dent.umich.edu. Contact: Lynn Monson, associate director of communications, at [email protected], or (734) 615-1971.
